Why Am I Bloated?
Bloating is generally understood as a mismatch between intestinal gas production, the ability of the digestive tract to distribute and clear that gas through coordinated propulsion, and the sensitivity of the gut to distension.
What is Bloating?
Bloating refers to a sensation of abdominal fullness, pressure, or swelling that commonly occurs after eating.
While it is often attributed simply to “gas,” bloating frequently reflects disruptions in how food is digested, fermented, and moved through the gastrointestinal tract.
In gastroenterology, bloating is considered a subjective sensation of abdominal fullness, while abdominal distension refers to a measurable increase in abdominal girth.
Many individuals experience bloating even when visible abdominal distension is minimal.
A Different Way to Understand Bloating
Bloating is often explained as a simple problem of excess intestinal gas. While gas production can certainly play a role, the physiology of bloating is usually more complex.
From a digestive physiology perspective, bloating often reflects a mismatch between:
how much gas is produced through fermentation
how effectively that gas is moved through the intestine
how sensitive the digestive tract is to distension
When these processes become poorly coordinated, normal digestive activity can produce sensations of pressure, fullness, or discomfort.
The Physiology of Post-Meal Bloating
After eating, several coordinated processes occur throughout the digestive tract.
Food enters the stomach, where digestion begins and downstream motility signals are generated. The small intestine continues to break down and absorb nutrients. Meanwhile, intestinal microbes ferment undigested nutrients and produce gases such as hydrogen, methane, and carbon dioxide. Most microbial fermentation normally occurs in the large intestine (colon), although fermentation may also occur in the small intestine when fermentable nutrients arrive there in significant amounts.
At the same time, coordinated muscular contractions move digestive contents forward through the gastrointestinal tract.
When these processes function normally, gas is distributed and cleared efficiently.
However, when digestion, fermentation, propulsion, or sensory signaling become disrupted, gas and luminal distension may accumulate and lead to bloating.
Different Patterns of Bloating
Not all bloating occurs in the same pattern. The timing of symptoms can sometimes provide clues about the underlying digestive processes involved.
Post-Meal Bloating
Bloating that occurs shortly after eating often reflects events occurring in the upper digestive tract, particularly the stomach and small intestine.
Potential contributing factors may include:
delayed gastric emptying
impaired stomach accommodation after meals
rapid delivery of poorly digested nutrients into the intestine
early fermentation of carbohydrates in the small intestine
heightened sensitivity to stomach or intestinal distension
In these situations, symptoms typically appear within minutes to an hour after eating.
Bloating That Worsens Throughout the Day
Some individuals notice that abdominal distension gradually increases as the day progresses, even if early meals are tolerated reasonably well.
This pattern may reflect processes occurring further along the digestive tract, including:
progressive accumulation of intestinal gas
slower intestinal propulsion
constipation or delayed transit
increased fermentation in the colon
difficulty clearing gas through normal intestinal movement
Because fermentation and gas production continue throughout the day, bloating may become more noticeable in the afternoon or evening.
Overlapping Patterns
In many cases, both patterns may occur together. For example, impaired digestion in the upper gastrointestinal tract may deliver excess nutrients to intestinal microbes. Carbohydrates that escape digestion may undergo fermentation, while undigested proteins may undergo putrefaction.
Both processes can generate gases and other metabolic byproducts that contribute to intestinal distension and the sensation of bloating later in the digestive process. In some individuals, microbial metabolites produced during fermentation or putrefaction may also influence intestinal motility and sensory signaling, further contributing to bloating symptoms.
For this reason, understanding the timing and pattern of bloating symptoms can provide useful clues about where digestive function may be disrupted.
Key Factors That Influence Bloating
Bloating rarely results from a single cause. Instead, it often reflects disruption in one or more systems that normally coordinate digestion, fermentation, and intestinal propulsion. Several key factors influence whether gas accumulates and produces symptoms.
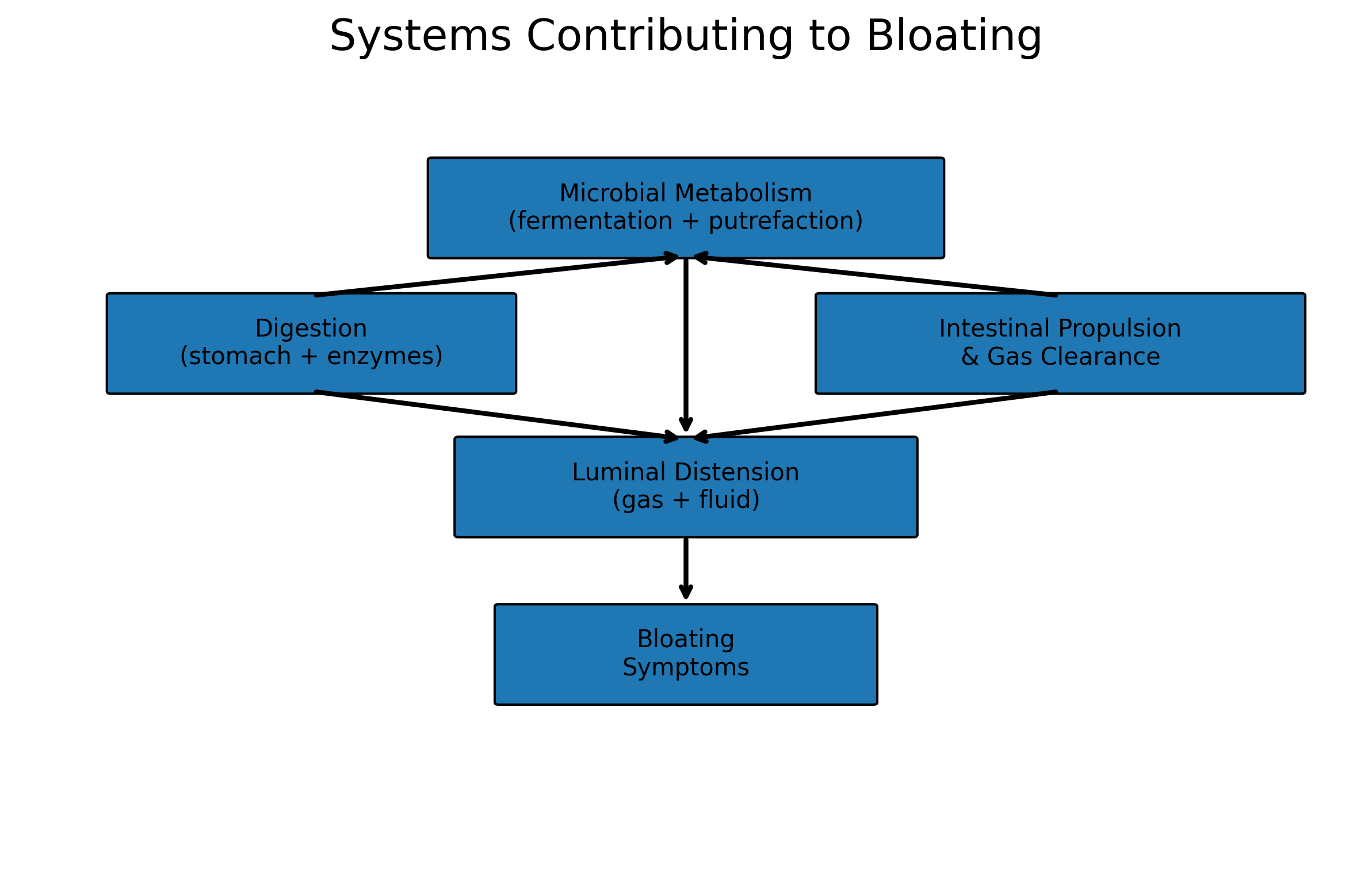
Figure: Systems contributing to bloating
Bloating often reflects the interaction between digestion, microbial metabolism (fermentation and putrefaction), intestinal propulsion, and the accumulation of gas and fluid within the intestinal lumen
Microbial Gas Production
Microorganisms within the digestive tract metabolize undigested nutrients through microbial processes such as fermentation and putrefaction. Fermentation typically occurs when microbes break down carbohydrates, while putrefaction occurs when microbes metabolize proteins that escape digestion.
When undigested proteins reach intestinal microbes, they may undergo putrefaction, a microbial process that produces sulfur-containing gases such as hydrogen sulfide along with other metabolic byproducts. These compounds often contribute to the characteristic odor associated with intestinal gas and may influence intestinal signaling and motility. In contrast, fermentation of carbohydrates typically produces gases such as hydrogen, methane, and carbon dioxide, which are largely odorless.
While microbial metabolism is a normal and important part of digestion, certain situations may increase gas production.
These may include:
diets high in fermentable carbohydrates (FODMAPs)
incomplete digestion of carbohydrates, fats, or proteins
enzyme deficiencies or digestive insufficiency
alterations in microbial composition
small intestinal bacterial overgrowth (SIBO)
When larger amounts of undigested nutrients reach intestinal microbes, microbial metabolism increases. Carbohydrates may undergo fermentation, while proteins may undergo putrefaction, generating gases and metabolic byproducts that contribute to luminal distension and the sensation of bloating.
Intestinal Propulsion and Gas Clearance
The digestive tract normally distributes and clears gas through coordinated muscular contractions known as intestinal propulsion.
When intestinal motility functions efficiently, gas produced during fermentation is moved along the digestive tract and eventually eliminated. Healthy individuals typically pass intestinal gas approximately 10–20 times per day, reflecting normal microbial fermentation and gas clearance.
Discomfort associated with bloating primarily arises when gas and fluid cause intestinal distension, which activates stretch-sensitive nerve endings within the intestinal wall. In individuals with increased visceral sensitivity, even normal levels of distension may produce noticeable pressure or discomfort.
However, when propulsion slows or becomes poorly coordinated, gas may accumulate within the intestine and contribute to the sensation of bloating.
This is one reason individuals with constipation or slow intestinal transit frequently experience abdominal bloating.
Healthy individuals typically tolerate normal levels of intestinal gas without discomfort. Symptoms often arise not from excessive gas production alone, but from altered gas distribution, impaired propulsion, or increased visceral sensitivity.
Luminal Factors and Osmotic Effects
The composition of intestinal contents can also influence bloating.
Certain carbohydrates draw water into the intestine through osmotic effects. This additional fluid, combined with fermentation gases, may increase intestinal distension.
Examples include:
high FODMAP foods
poorly absorbed carbohydrates
sugar alcohols
Luminal contents may also interact directly with the intestinal lining. Nutrients, microbial metabolites, bile acids, and other luminal factors can influence intestinal cells, nervous system signaling, secretion, and motility. These interactions may further affect how gas and fluid are handled within the digestive tract.
Many luminal signals ultimately influence intestinal propulsion by interacting with the enteric nervous system, which continuously integrates chemical signals, microbial metabolites, and mechanical distension within the intestinal lumen to regulate digestive motility.
Visceral Sensitivity
Not all bloating results from excessive gas production.
In some individuals, the digestive tract becomes more sensitive to normal levels of intestinal distension. This phenomenon is known as visceral hypersensitivity.
When visceral sensitivity is increased, even relatively small amounts of gas or fluid within the intestine may produce noticeable sensations of pressure, fullness, or discomfort. In these situations, symptoms may occur even when overall gas production remains within a normal range. This mechanism is commonly observed in conditions such as irritable bowel syndrome (IBS).
Chemical irritation within the digestive tract may also lower the threshold at which intestinal sensory nerves respond to mechanical stimuli. Substances present within the intestinal lumen — including microbial metabolites, bile acids, and other luminal compounds — can sensitize the intestinal lining. As a result, normal levels of distension may be perceived as uncomfortable or painful more easily than they otherwise would be.
Because visceral sensitivity is shaped by ongoing communication between the gut, the nervous system, and the abdominal tissues themselves, it is not necessarily fixed. In clinical practice, therapies such as acupuncture and visceral manipulation are often observed to reduce abdominal tenderness, digestive sensitivity, and bloating. These changes likely reflect modulation of sensory signaling, autonomic tone, and the mechanical environment surrounding the digestive organs.
Nervous System Regulation
The digestive tract is regulated by a complex network of nerves known as the enteric nervous system, which works in close coordination with the brain and autonomic nervous system.
These neural systems continuously monitor conditions within the digestive tract and help coordinate:
intestinal motility
digestive secretions
visceral sensitivity
the movement and distribution of intestinal gas
Signals from the gut travel to the spinal cord and brain through sensory nerve pathways, while descending signals from the brain influence digestive activity through sympathetic and parasympathetic pathways.
Because of this two-way communication, factors such as stress, autonomic balance, inflammation, luminal signals, and mechanical forces within the abdomen can influence how digestive propulsion is regulated and how digestive sensations are perceived.
In other words, the nervous system acts as a central coordinator of digestive motility.
Because so many factors influence the nervous system control of the gut, clinicians generally aim to use interventions that produce reliable and reproducible improvements in digestive coordination. In my clinical experience, therapies that directly influence the abdominal organs and surrounding tissues — such as acupuncture and visceral manipulation — are among the most consistently helpful approaches for supporting coordinated digestive propulsion. These interventions may influence sensory signaling, autonomic balance, and the mechanical environment of the digestive organs, all of which interact with the nervous system regulation of gut motility.
For this reason, these therapies are commonly incorporated into treatment plans when working to improve persistent bloating and other functional digestive symptoms.
Bringing These Factors Together
Digestion, microbial metabolism, intestinal propulsion, and nervous system signaling are closely interconnected processes. Bloating often reflects a disruption in the coordination of these systems rather than a single isolated cause.
For example, reduced digestive efficiency may allow larger amounts of nutrients to reach intestinal microbes. Increased fermentation may then generate additional gas. If intestinal propulsion is also slowed, gas may accumulate more easily within the digestive tract. At the same time, heightened visceral sensitivity may amplify the perception of intestinal distension.
Because these processes influence one another, symptoms such as bloating frequently arise from a combination of factors rather than a single mechanism.
Understanding which aspects of digestion, microbial activity, intestinal propulsion, and nervous system regulation are most affected can help guide more targeted approaches to improving digestive comfort.
Symptom-Focused Products for Gas
Some over-the-counter products are designed to reduce symptoms related to intestinal gas. These enzyme products (such as alpha-galactosidase), gas-reducing agents such as simethicone, and adsorbent substances such as activated charcoal. These products may provide temporary relief for some individuals by reducing gas formation or altering how gas behaves within the intestine. However, they typically address only one part of the overall process — gas itself.
Because bloating often reflects broader issues involving digestion, intestinal propulsion, microbial metabolism, and nervous system regulation, symptom-focused products may not fully resolve bloating when the underlying coordination of digestive function remains disrupted.
For this reason, improving the overall coordination of digestion and intestinal propulsion is often an important part of achieving more consistent relief from bloating.
When to Seek Assessment
Occasional bloating can occur as part of normal digestion. However, persistent or recurrent bloating is not typically a normal digestive experience and often reflects underlying disruptions in digestive coordination.
Bloating may be associated with factors such as altered digestion, increased microbial fermentation, impaired intestinal propulsion, heightened visceral sensitivity, or changes in nervous system regulation of the gut.
Because these mechanisms can vary significantly from person to person, persistent bloating often requires individualized assessment to determine which aspects of digestive function are contributing most strongly to symptoms.
Certain accompanying symptoms — such as persistent abdominal pain, unexplained weight loss, significant changes in bowel habits, or difficulty tolerating foods — should always be evaluated.
Even in the absence of these warning signs, persistent bloating that occurs alongside other digestive symptoms — such as reflux, constipation, diarrhea, excessive gas, or ongoing abdominal discomfort — often indicates that digestive function is not operating optimally and may benefit from further assessment.
A careful evaluation of overall digestive function can help identify factors such as altered motility, microbial imbalance, digestive insufficiency, or nervous system influences that may contribute to ongoing symptoms. Evaluating these aspects of gut function can help inform the most appropriate steps to address the underlying causes of bloating.
In many cases, improving digestive comfort involves restoring the normal coordination between digestion, microbial activity, intestinal propulsion, and nervous system regulation within the gut.